Montreal doctors, advocates call out possible racial bias in pulse oximeters
Posted February 21, 2022 10:54 am.
Last Updated February 21, 2022 10:56 am.
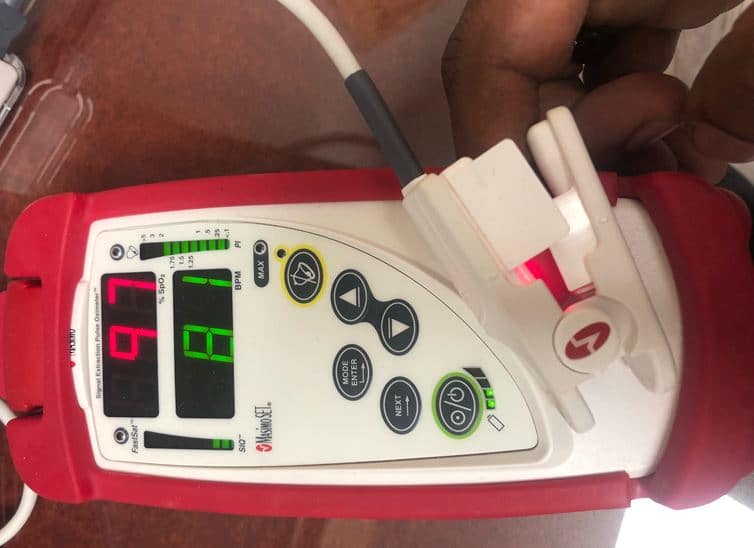
The pulse oximeter, usually put on a patient’s fingertip, estimates the amount of oxygen in the blood without having to draw a blood sample. It’s often used to treat patients with COVID-19, but multiple factors can affect the accuracy of its reading, like fingernail polish, poor circulation, skin thickness, but one factor has left some in disbelief – a recent report showing that readings may be inaccurate in patients with darker skin.
“I think it’s definitely a cry for more culturally sensitive and culturally adapted medicine from coast-to-coast,” said Dr. Frantz-Daniel Lafortune, Quebec representative, Black Physicians of Canada.
Invented in the 1970s, it’s said to have revolutionized hospital care, showing second by second what’s happening with oxygen in a person’s blood.
“This parameter is really key in saying, ‘would you give oxygen to this patient or would you give some other drugs to treat them?’ It is extremely concerning that that this thing could be happening,” said Dr. Frantz-Daniel Lafortune .
“There can be inaccuracies related to the skin tone that a patient has,” explained Dr. Saleem Razack, Director, Office of Social Accountability and Community Engagement, McGill University. “There’s five classifications or gradations of skin tone that that we talk about in medicine from lightest to darkest, and at the darker end of the skin tones with many pulse oximeters there can be a difference of two or three percentage points in the measurement of oxygen in the blood.”
In many cases, the FDA says that the difference may be small, however, there is a risk that an inaccurate measurement may result in unrecognized low oxygen saturation levels.

Pulse oximeter (CREDIT: Dr. Christopher Labos)
Dr. Razack says, despite the small percentage difference, it’s still important to be aware of the device’s limitations. “Particularly in my setting, [it’s] been about making sure that people are well trained to understand that this exists and to act accordingly.”
A 2020 study by The New England Journal of Medicine, titled ‘Racial Bias in Pulse Oximetry Measurement,’ found that the pulse oximeter overestimated oxygen levels 3.6 per cent of the time in white patients – and for Black patients, overestimated nearly 12 per cent of the time.
“Members of vulnerable communities, marginalized communities, Indigenous, Black communities, [should] really consider joining one of the patients committee of the hospital where you go, where you get your care,” said Seeta Ramdass, a patient advocate.
Many calling for people to get involved in their own medical care and have their voices heard. That examples like the pulse oximeter are just one of many where there are disaprities between groups.
“As long as you use the service of the hospital and have had even a blood test there, you can contribute to the dialog and advocate for patients rights, advocate for your community to get optimal care,” explained Ramdass.
“I think it’s important to know and to be accurate so that you can sort of care for the patient to the best that you can,” added Dr. Razack.
“To adapt better our devices, our medical devices, to the patient that we treat, so we can better serve them. So we can better serve the ensemble of our society,” said Dr. Lafortune.”